Arkansas medicaid
Reports and Explainers
News and Updates
Arkansas chose to participate in the federal Medicaid program in 1970, expanding the state’s role in providing healthcare coverage to low-income children and their parents, pregnant women, individuals with disabilities, and other low-income populations. The Arkansas Medicaid program is overseen by the Arkansas Department of Human Services. The U.S Centers for Medicare and Medicaid Services ensures that the state’s plan complies with federal regulations.
The Arkansas Medicaid program has continued to evolve since its establishment, reducing the number of Americans without healthcare coverage. Arkansas has historically maintained some of the strictest income eligibility requirements for program enrollment based on many factors, including income, state residency, and disability status.
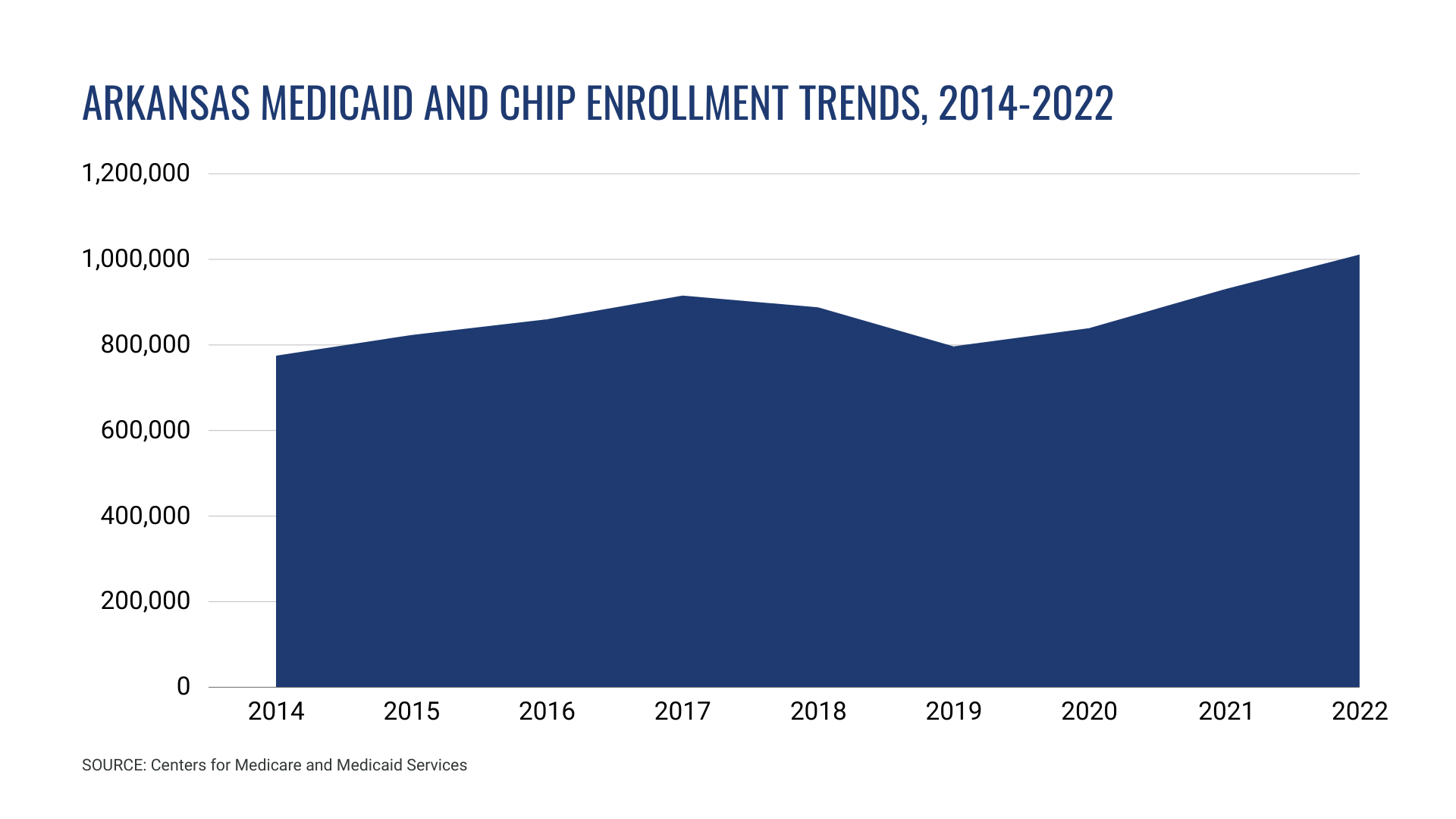
In 2014, Arkansas implemented a unique version of Medicaid expansion through the Arkansas Health Care Independence Program, currently known as Arkansas Health and Opportunity for Me (ARHOME). In addition to providing healthcare coverage to low-income, non-caretaker adults, the expansion of the Arkansas Medicaid program also resulted in reduced uncompensated care costs for hospitals, which helped Arkansas avoid the rural hospital closings experienced in neighboring states.
Financing for Medicaid is a shared responsibility between the state and federal governments based on a match rate. The rate varies based on states’ average per capita incomes, with lower-income states receiving greater federal assistance.
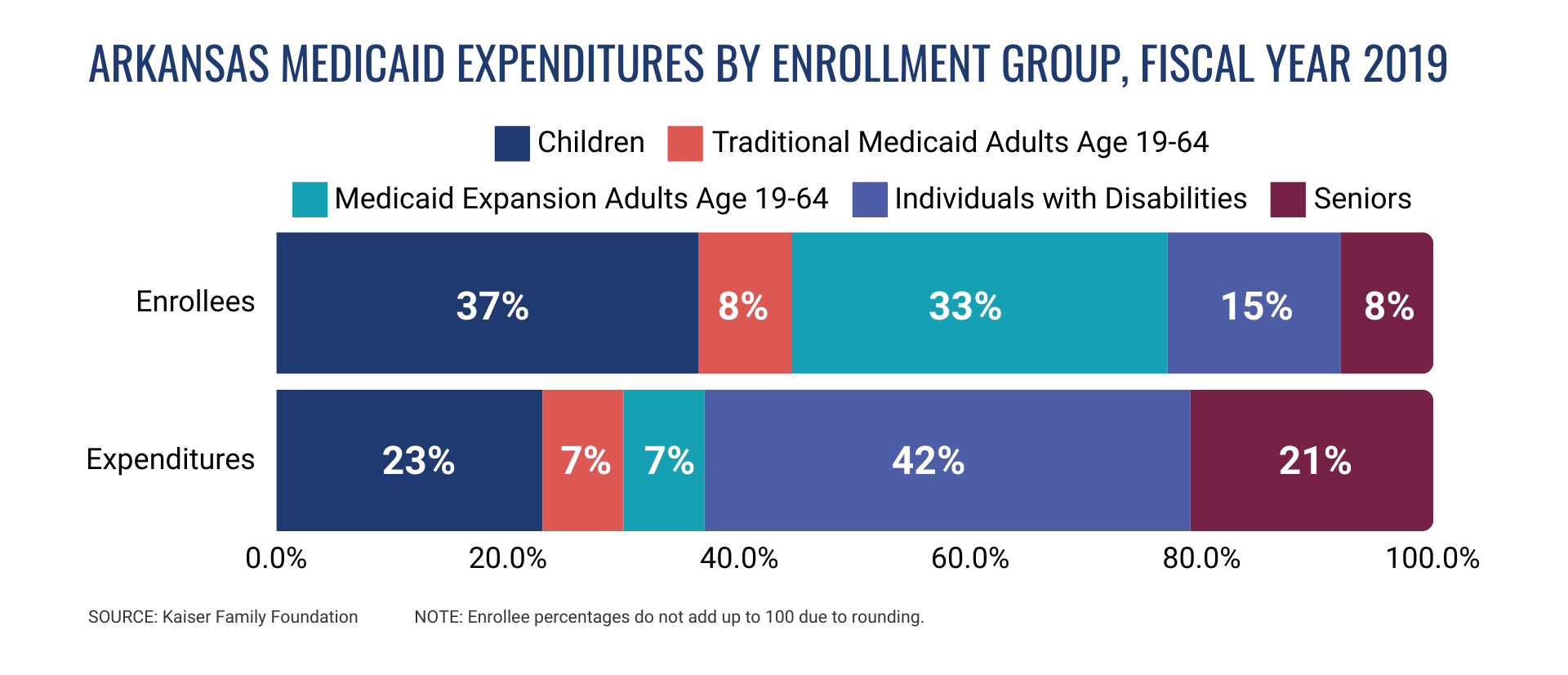
State and federal policymakers frequently explore changes to the Medicaid program, including efforts to rein in costs while also ensuring sufficient access to quality care. Amid 2025 federal budget discussions, Congress shows a clear intent to reduce federal expenditures on health care, shifting financial responsibility for Medicaid and other federal programs to the states and local communities.
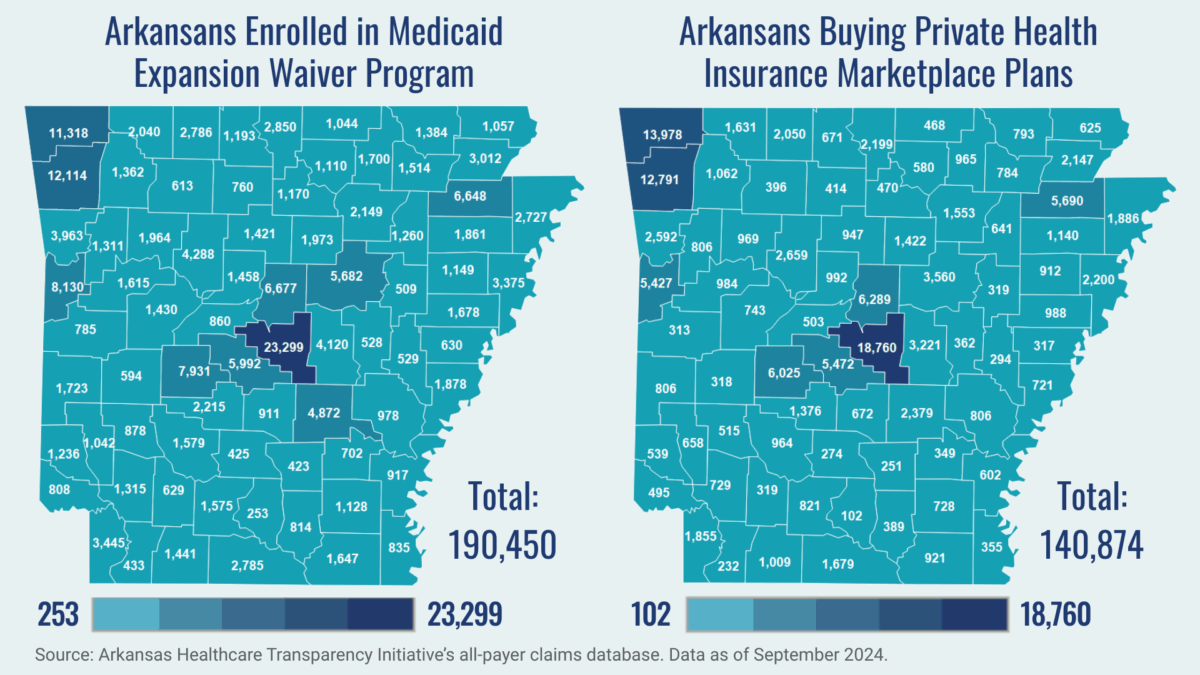
To better understand and estimate the potential impact of congressional budget decisions that reduce federal expenditures on Medicaid and other healthcare coverage programs, ACHI developed two maps that show enrollment data as of September 2024 for the state’s Medicaid expansion waiver program (Arkansas Health and Opportunity for Me, or ARHOME) and for Arkansans buying private insurance through the Health Insurance Marketplace.
A thorough understanding of Medicaid and its history is critical to better understand the impacts of proposed policy changes. ACHI’s Arkansas Medicaid Primer provides an overview of Medicaid in Arkansas, including its history, its financing structure, covered populations and benefits, and key policy considerations.














